
Context
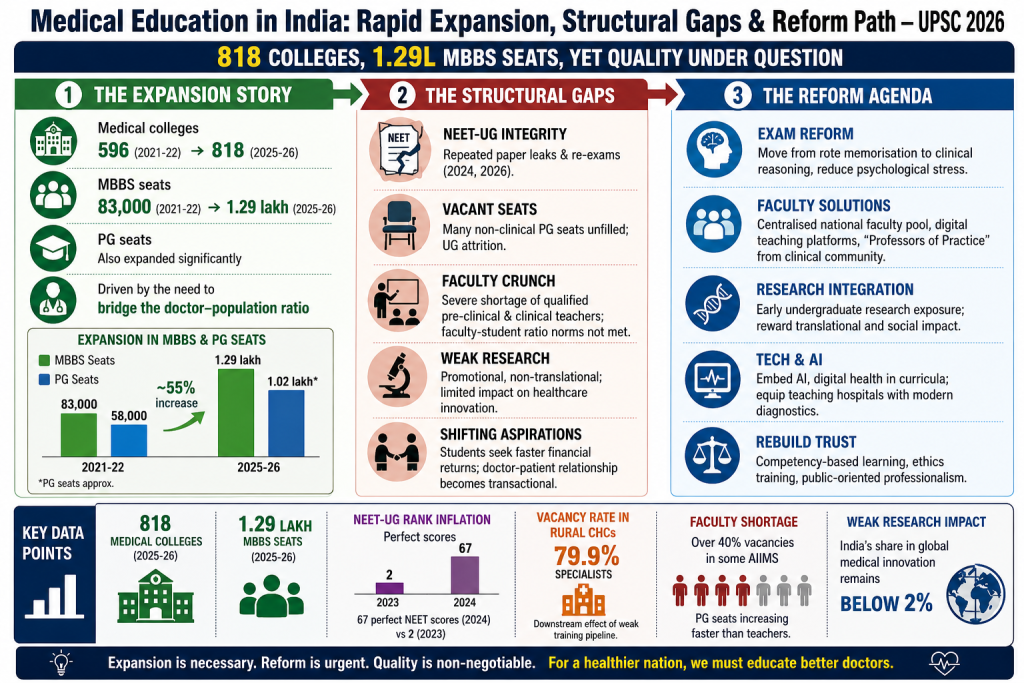
- India has witnessed rapid expansion in medical colleges and MBBS seats over the past decade. The cancellation of NEET-UG revived concerns regarding quality, transparency, and structural weaknesses in medical education.
Expansion of Medical Education in India
- Growth in Institutions and Seats
- The number of medical colleges increased from around 596 in 2021-22 to over 818 in 2025-26.
- MBBS seats expanded from nearly 83,000 to around 1.29 lakh nationwide.
- Postgraduate medical seats have also increased significantly across the country.
- Concerns regarding Expansion
- Rapid expansion has raised concerns regarding quality of medical training and institutional preparedness.
- Several undergraduate and postgraduate seats remain vacant, especially in non-clinical specialities.
- Mismatch between seat creation and student preferences reflects deeper structural issues.
Structural Issues in Medical Education
- Changing Aspirations among Students
- Long duration of medical education and increasing professional stress are reducing the appeal of the profession.
- Younger generations increasingly prefer careers offering quicker financial stability and work-life balance.
- The traditional prestige associated with the medical profession is gradually weakening.
- Changing Doctor–Patient Relationship
- Doctors are increasingly viewed within a transactional healthcare system rather than as unquestioned social figures.
- Rising accountability and public scrutiny have altered the nature of healthcare relationships.
- Declining public trust may affect morale within the medical profession.
- Limitations of NEET System
- NEET was introduced to ensure standardisation and transparency in medical admissions.
- Repeated paper leaks and re-examinations have raised concerns regarding examination integrity.
- Excessive reliance on rote learning limits assessment of higher-order clinical reasoning abilities.
- Faculty Shortages
- Medical institutions face severe shortages of qualified teaching faculty, especially in pre-clinical disciplines.
- Rapid expansion of colleges has outpaced availability of trained academic professionals.
- Existing faculty-student ratio norms remain difficult to achieve in practice.
- Weak Research Ecosystem
- Large sections of medical research remain non-translational and promotion-oriented.
- Much research output contributes little to healthcare delivery or scientific innovation.
- Weak integration of research culture limits innovation within medical education.
Need for Structural Reforms
- Reforming Examination and Assessment Systems
- Medical entrance examinations should focus upon clinical reasoning and cognitive skills rather than rote memorisation.
- Examination systems should reduce psychological stress among aspirants.
- Outcome-based assessment models should replace excessive checklist-oriented evaluation.
- Addressing Faculty Constraints
- A centralised national faculty pool can optimise faculty availability across institutions.
- Digital teaching platforms can improve access to experienced educators nationwide.
- Experienced clinicians should be integrated as “Professors of Practice” within medical institutions.
- Promoting Research and Innovation
- Medical education should prioritise translational and socially relevant research.
- Undergraduate students should receive early exposure to research and inquiry-based learning.
- Research training should become an integral component of medical assessment systems.
- Integrating Technology and AI
- Artificial Intelligence and digital health technologies are becoming central to modern healthcare systems.
- Medical curricula should introduce AI and digital health education at early stages.
- Teaching hospitals should be equipped with modern diagnostic and technological infrastructure.
- AI should function as an aid to strengthen clinical judgment rather than replace doctors.
Way Forward
- India should shift focus from numerical expansion towards quality-oriented medical education reforms.
- Regulatory frameworks should prioritise competency-based learning and practical skill development.
- Faculty shortages should be addressed through flexible institutional and technological solutions.
- Medical education should strengthen ethical professionalism and rebuild public trust in healthcare systems.
- Stronger integration of research, technology, and clinical reasoning can prepare doctors for future healthcare challenges.
Conclusion
- India has largely addressed the challenge of expanding medical education capacity, but quality concerns remain significant. Sustainable healthcare advancement will depend upon producing competent, compassionate, and technologically skilled doctors capable of addressing future national health needs.

