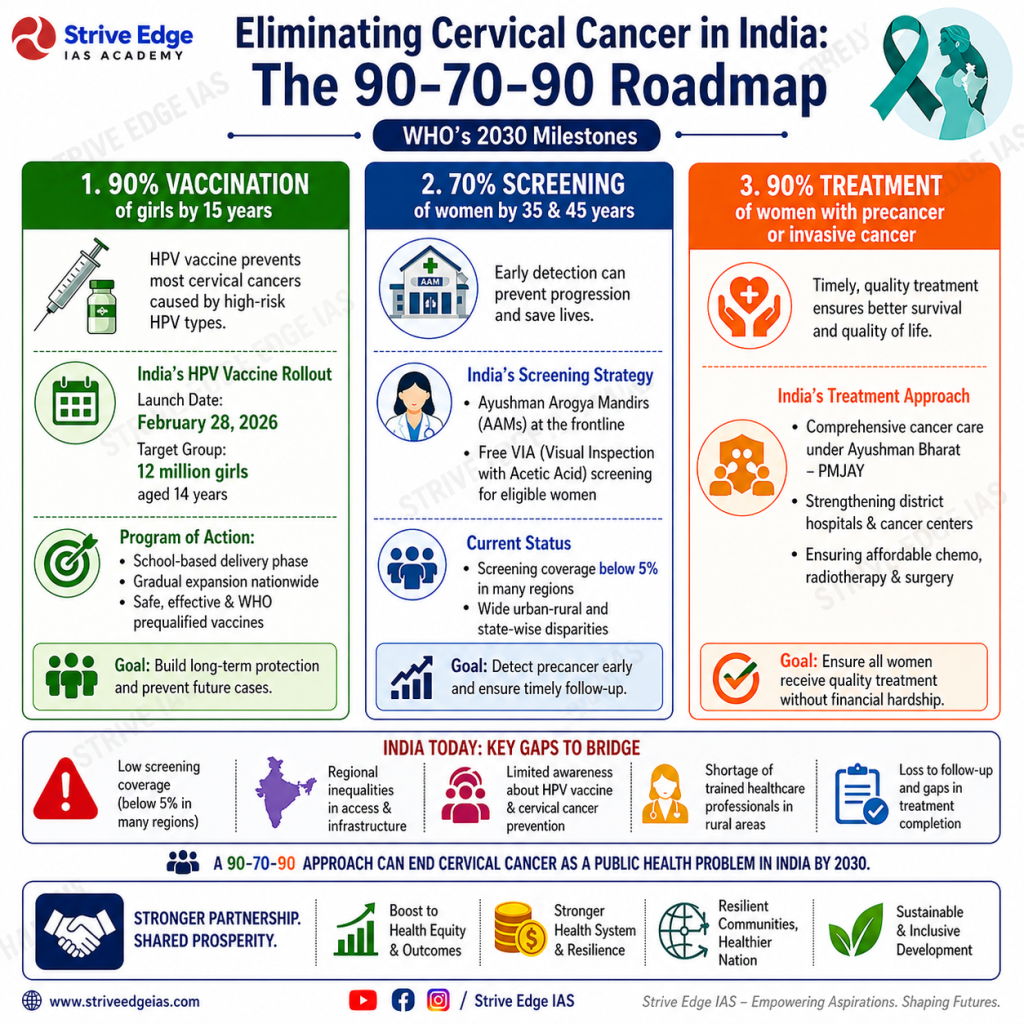
Context: Cervical cancer remains a major public health challenge, especially in low and lower-middle-income countries, with India bearing a significant share of the global burden. The WHO’s global initiative (2020) aims to eliminate cervical cancer as a public health problem, with India committing to this vision through policy and vaccination programmes.
About Cervical Cancer
- Disease Burden: Cervical cancer is the second most common cancer among women in India, with nearly 1 lakh new cases annually and about 50,000 deaths.
- Cause: Persistent infection with high-risk Human Papillomavirus (HPV) is the primary cause.
- Natural History: The disease has a long precancerous phase (10–15 years), allowing early detection and treatment.
- Preventability:
- Primary Prevention: HPV vaccination
- Secondary Prevention: Screening through Pap smear or HPV tests
- Thus, the cervical cancer is one of the most preventable yet highly prevalent cancers, reflecting gaps in public health delivery.
How Prevention Framework Ensures Health Inclusion
- HPV Vaccination Impact: A single dose provides 85–90% protection against major cancer-causing strains.
- Global Evidence: Countries like Australia, UK, Sweden, and Canada have reported significant declines in cervical cancer incidence after vaccination programmes.
- Accessibility and Equity: India’s National HPV Vaccination Campaign (2026) aims to provide free vaccination to adolescent girls, improving access for vulnerable populations.
- Health Equity Dimension: Preventive care reduces physical suffering, financial burden, and gender-based health disparities.
- These initiatives promotes inclusive public health by ensuring that prevention reaches those most at risk.
Issues Associated
- Low Screening Coverage: Despite programmes, screening coverage in India remains below 5%, limiting early detection.
- Infrastructure Constraints: Lack of laboratory capacity, trained manpower, and outreach systems restricts large-scale screening.
- Poor Follow-Up Compliance: Women identified as positive often do not return for confirmatory tests or treatment.
- Awareness Deficit: Limited public awareness about HPV vaccination and screening reduces uptake.
- Health System Gaps: Outreach programmes remain fragmented and insufficient to cover large populations.
- These limitations highlight that prevention requires not just policy, but strong delivery systems and behavioural change.
Conclusion
- Cervical cancer elimination represents a rare convergence of scientific possibility and public health opportunity, where effective prevention tools already exist. Achieving WHO targets will require sustained efforts in vaccination, screening, and treatment, supported by awareness and system strengthening.
- A coordinated approach can transform cervical cancer from a major killer into a largely preventable and rare disease, advancing both women’s health and national development goals.

